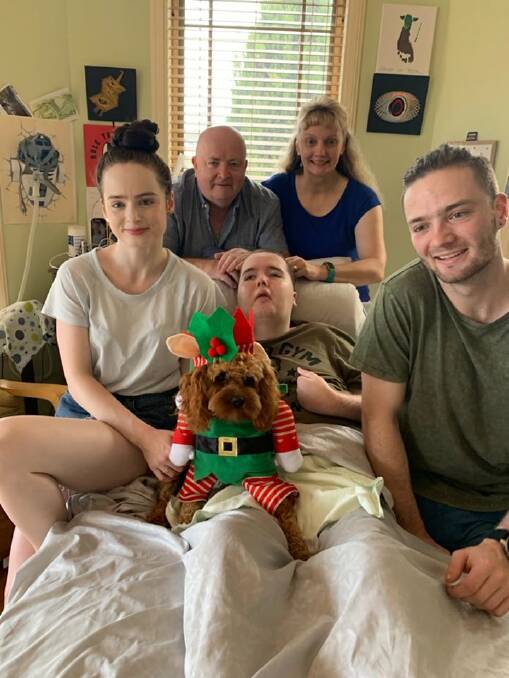
Mick and Suzanne Reynolds, whose son Kieran suffered severe brain damage during a procedure at Bega Hospital in 2015, have vowed to continue to advocate for improved processes and procedures at rural and regional hospitals.
Subscribe now for unlimited access.
$0/
(min cost $0)
or signup to continue reading
On Monday, September 9 their story was aired on Four Corners.
"It was extremely confronting to see our boy on the big screen but what stood out for me was that no one from Bega (Hospital) had commented. There was no management comment from Southern NSW Local Health District (SNSWLHD)," Ms Reynolds said.
In 2015 Kieran was a lively Year 9 student at Lumen Christi with his future before him. Today he spends his time on a special pressure bed, he is blind, unable to talk and a quadriplegic, requiring 24-hour care.
In December 2018 the SNSWLHD admitted liability for Kieran's brain damage which occurred when an endotracheal tube was incorrectly positioned resulting in oxygen going into Kieran's stomach and not his lungs for 20 minutes.
Read more here: Hospital admits liability for Tura boy's brain damage
It should not be the case that your postcode can dictate whether your next visit to hospital is your last.
- Shannon Reynolds
Ms Reynolds said that as parents and nurses they wanted to do anything that would prevent this happening again.
Mr Reynolds said he was concerned that despite the area having a new hospital, "there is not adequate staffing or appropriate staffing" something he believes is due to government funding.
Both the president of the Rural Doctors of Australia Association (RDAA) Dr Adam Coltzau and the chair of the National Rural Health Alliance Tanya Lehmann have pointed to funding issues.
"We know there is a large gap in health funding and the outcomes for rural and remote people. The provision of timely and high quality health care is complex and requires significant long-term attention and political will by all levels of government," Ms Lehmann said.
Dr Coltzau said the issues raised demonstrated lack of resourcing in regional and rural hospitals, both in terms of the available health workforce and equipment.
We know there is a large gap in health funding and the outcomes for rural and remote people.
- Tanya Lehmann, chair of the National Rural Health Alliance
"The National Rural Generalist Training Pathway, currently in development, holds real promise to deliver more of the next generation of doctors to rural communities, trained in the advanced skills that will be required of them. This includes Emergency skills in addition to primary care and other advanced skills. But this pathway alone will not be the panacea," Dr Coltzau said.
He said that that the retrieval system was not always a perfect system with multiple demands on retrieval aircraft, or crew shortages, or bad weather preventing them from getting to a particular location.
"Governments and policy-makers need to ensure that, in decisions made around resourcing regional or rural hospitals and retrieval services, all these issues are taken into account," Dr Coltzau said.
Kieran's sister Shannon said she felt she had an opportunity to use her unique perspective to advocate for change.
"My parents, both nurses, subsequently retired early in order to meet my brother's 24/7 care needs. Unfortunately, my story is not uncommon nor will it be the last, unless something is done about rural and regional healthcare in Australia," Ms Reynolds said.
"Chronic underfunding, poor oversight and a lack of government led incentives to encourage medical practitioners to live and work in rural and regional Australia means that basic medical procedures can result in catastrophic, life-altering consequences for a patient and their loved ones," she added.
Kieran's mum Ms Reynolds said that it had taken a terrible toll on both her and husband Mick but they wanted to continue to advocate for improvements and were keen to work with the SNSWLHD to assist in any way they could.

